Hair shedding can sometimes increase suddenly and cause understandable concern. One of the most common reasons for this type of shedding is a condition known as telogen effluvium. In this condition, a larger than usual number of hair follicles shift into the resting phase of the hair growth cycle.
Because hair follicles normally operate independently, only a small proportion of hairs are in the resting stage at any given moment. In telogen effluvium, however, many follicles enter this stage at roughly the same time. The result is increased hair shedding several months later.
Although the shedding can be noticeable, the follicles themselves usually remain capable of producing new hair.
The normal balance of the hair cycle
To understand telogen effluvium, it is useful to recall how the hair growth cycle normally works.
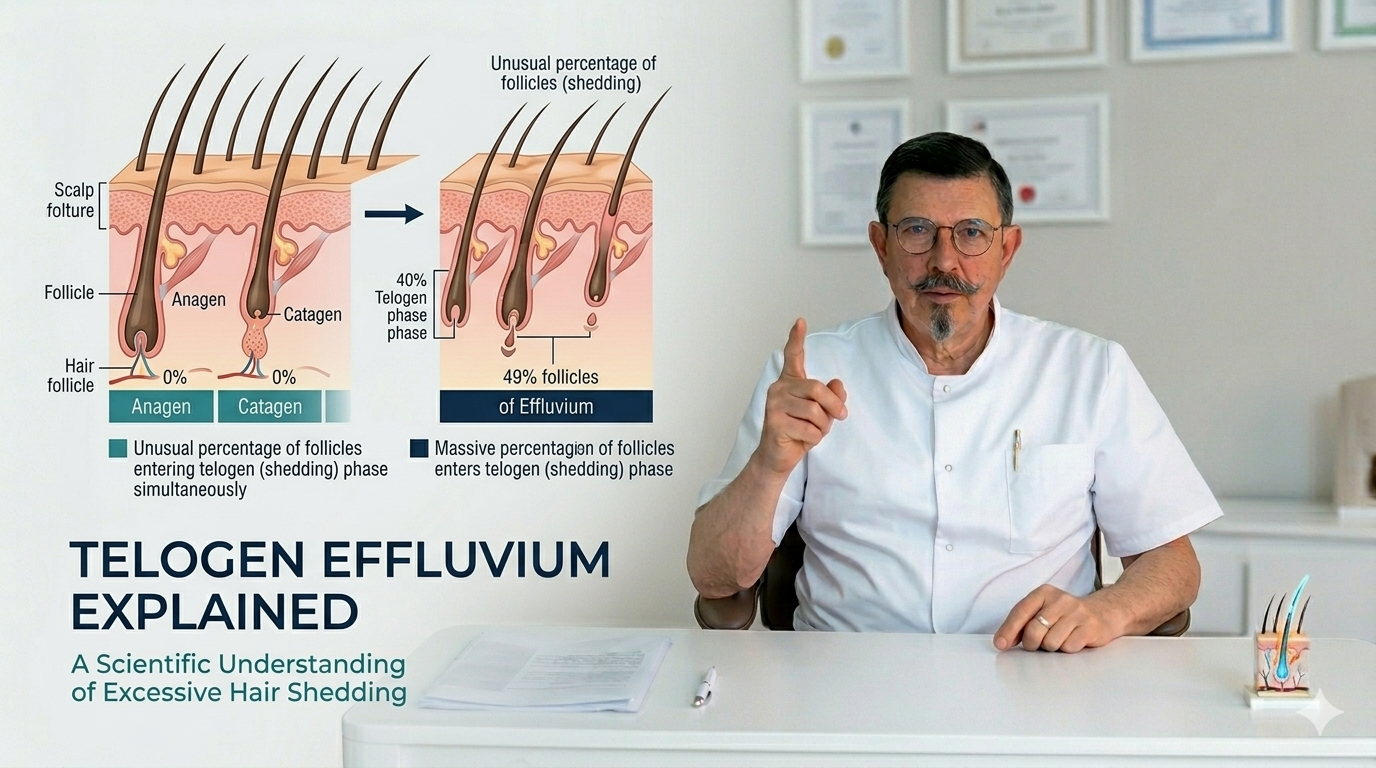
Each follicle moves through three main phases. The anagen phase is the active growth stage. The catagen phase is a short transition period during which growth stops. The telogen phase is the resting stage, after which the hair sheds and a new cycle begins.
In a healthy scalp, most hairs are in the growth phase. Only a small percentage are in the resting phase at any given time. This balance allows hair shedding to occur gradually and without noticeable thinning.
Telogen effluvium develops when this balance is temporarily disrupted.
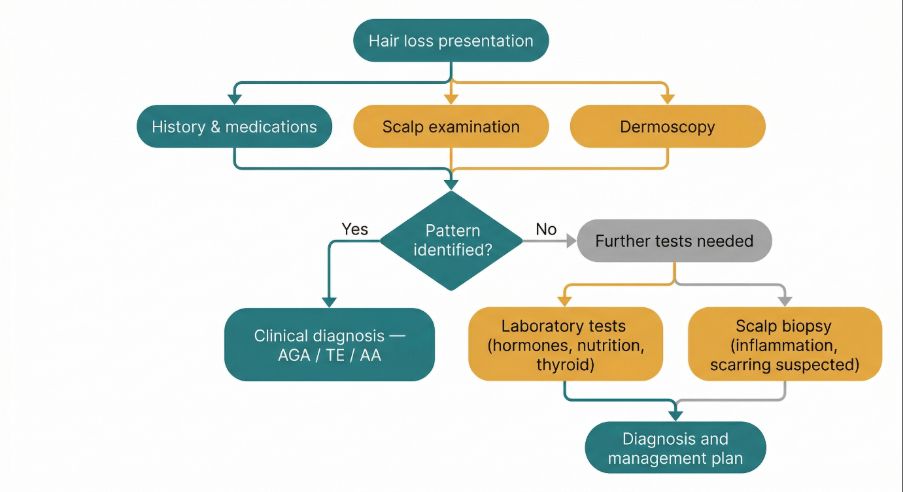
What happens during telogen effluvium
In telogen effluvium, a significant number of follicles prematurely enter the resting phase of the hair cycle.
Because the resting phase typically lasts several months, the increased shedding does not occur immediately after the triggering event. Instead, hair shedding usually becomes noticeable two to three months later.
When these resting hairs are eventually released, the individual may notice increased hair fall during washing, brushing, or styling.
Despite the increase in shedding, the follicles themselves usually remain intact and capable of producing new hair during the next growth cycle.
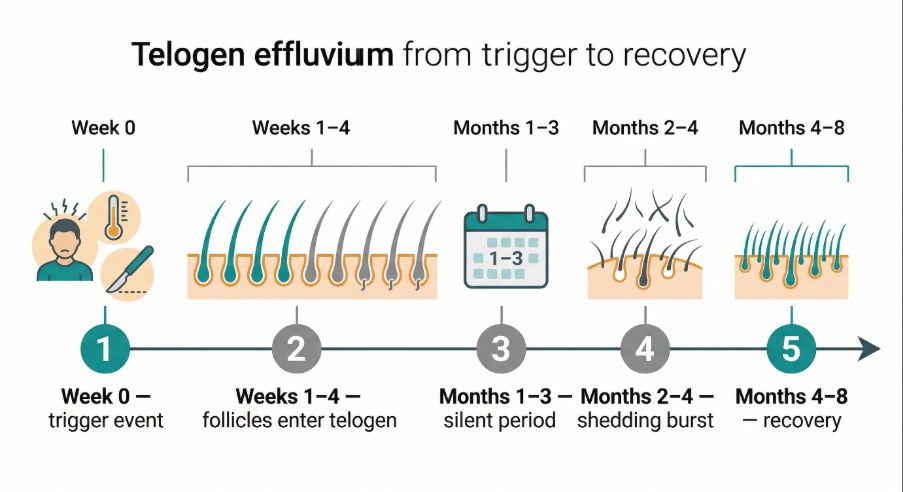
Common triggers
Telogen effluvium often develops after a significant physiological or emotional stress on the body.
Several events can act as triggers. These include severe illness, high fever, surgery, major psychological stress, or significant hormonal changes.
Childbirth is another well recognised trigger. After pregnancy, some women experience increased hair shedding as the hair cycle adjusts to changing hormonal levels.
Certain medications, nutritional deficiencies, or rapid weight loss may also influence the hair cycle and contribute to temporary shedding.
In many cases, the triggering event may have occurred several months before the shedding becomes noticeable.
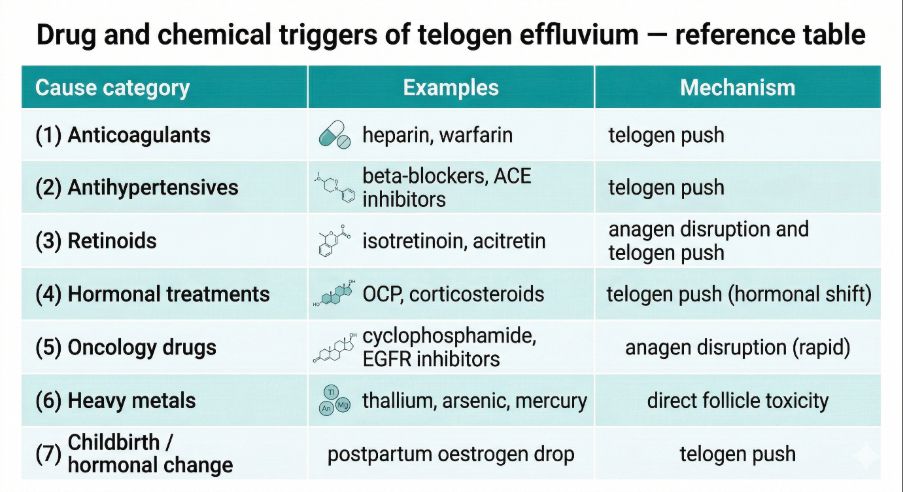
Certain medications are a recognised trigger. Drug categories known to precipitate telogen effluvium include anticoagulants such as heparin and warfarin, antihypertensive agents including beta-blockers, retinoids, hormonal treatments, and oncology drugs. Cytotoxic chemotherapy agents can also directly disrupt the anagen phase. In most medication-related cases, shedding begins two to four months after the drug was introduced, reflecting the duration of the telogen phase.
Chemical exposures are an additional cause. Heavy metals including thallium, arsenic, and mercury are well-established triggers for hair cycle disruption, with exposure occurring through occupational contact, contaminated environments, or ingestion. Industrial solvents and harsh chemical hair treatments may also impair follicle function and precipitate shedding.
How telogen effluvium appears
The hair shedding associated with telogen effluvium is usually diffuse, meaning it occurs across the entire scalp rather than in a specific pattern.
Individuals may notice more hairs than usual on the pillow, in the shower drain, or on a hairbrush. The hairline typically remains unchanged, and the scalp does not usually develop distinct bald patches.
Although shedding can appear dramatic, the scalp generally retains a large number of follicles capable of producing new hair.
Because the follicles are not permanently damaged, the condition is usually temporary.

Recovery of the hair cycle
Once the triggering factor has resolved, the hair growth cycle often gradually returns to its usual pattern.
As follicles re-enter the growth phase, new hairs begin to emerge from the scalp. These new hairs may initially appear short or fine but typically thicken over time as the growth cycle stabilises.
The process of recovery may take several months because hair grows slowly and the cycle of the follicle takes time to normalise.
In many individuals, hair density gradually improves as new growth replaces the hairs that were shed.
When shedding persists
In some cases, telogen effluvium can become prolonged.
If the underlying trigger remains present, or if multiple triggers occur over time, the disruption of the hair cycle may continue. This may lead to persistent shedding lasting longer than the typical recovery period.
Certain medical conditions, nutritional factors, or ongoing stress may contribute to prolonged disruption of the hair cycle.
Because many factors can influence hair shedding, persistent hair loss may require clinical evaluation to determine the underlying cause.
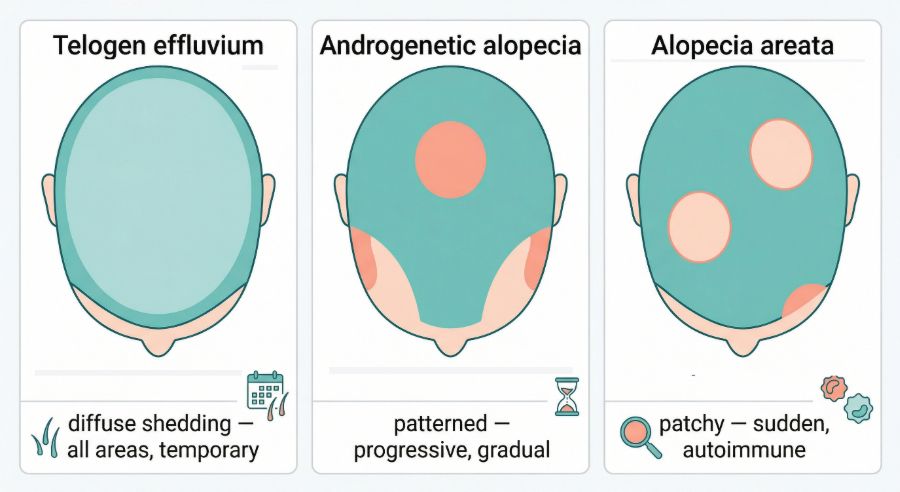
Distinguishing telogen effluvium from other types of hair loss
Telogen effluvium differs from several other forms of hair loss.
In androgenetic alopecia, hair follicles gradually shrink and produce thinner hair shafts over time. This process leads to patterned thinning rather than sudden shedding.
In alopecia areata, hair loss often occurs in well defined patches due to immune system activity affecting the follicles.
Telogen effluvium, by contrast, involves increased shedding across the entire scalp while the follicles remain structurally intact.
Recognising these differences is important when evaluating hair loss.
A broader perspective
Telogen effluvium represents a temporary disturbance of the hair growth cycle rather than permanent damage to the hair follicle.
Because many follicles enter the resting phase simultaneously, the shedding may appear dramatic. However, the follicles themselves usually remain capable of producing new hair.
As the body recovers from the triggering event, the hair cycle often returns to its usual rhythm and new hair growth gradually restores coverage of the scalp.
Understanding this process can help place episodes of increased hair shedding into a biological context and explain why recovery often takes several months.
Author: Dr. Priya Goswami
Medical review: Dr. Denis Broun
Next step
If you notice coverage changes without increased shedding, confirm what process is occurring.
Take the Hair Assessment to have a physician review your pattern, identify whether miniaturization is present, and determine appropriate staging and next steps.
Add Comment