Male pattern hair loss is the most common form of hair thinning in men. It develops gradually and usually follows a characteristic pattern involving the temples and the crown of the scalp. In medical terms, this condition is known as androgenetic alopecia.
The process does not occur suddenly. It develops over many years through changes in the behaviour of hair follicles. These changes are influenced by genetic factors and by the way certain hormones interact with the follicles.
Understanding the biological mechanisms behind male pattern hair loss helps explain why the condition progresses slowly and why it affects specific areas of the scalp.
The role of genetics
Genetics plays a central role in male pattern hair loss. Some individuals inherit hair follicles that are more sensitive to hormonal signals than others.
This inherited sensitivity influences how follicles respond over time. In people who are genetically predisposed, certain follicles gradually change their behaviour during the hair growth cycle.
Not everyone with a genetic predisposition develops noticeable hair loss at the same age. The timing and speed of progression vary between individuals and families.
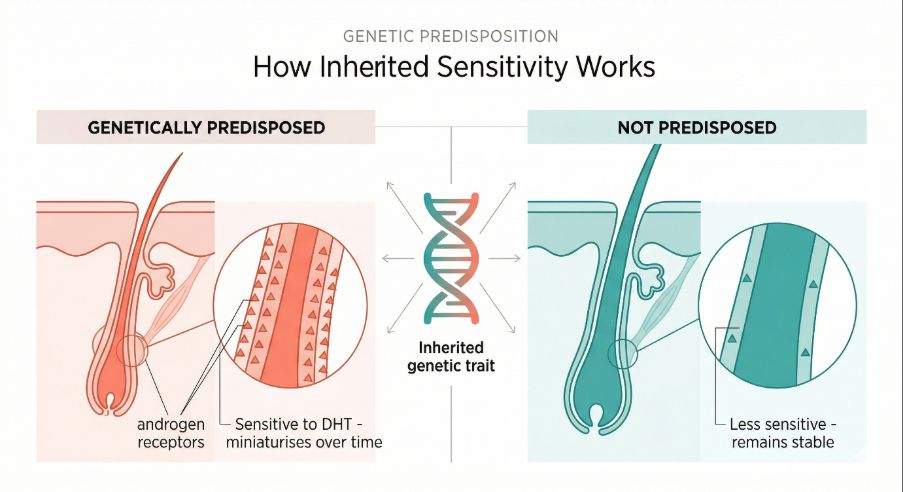
Hormonal influence on the follicle
Hair follicles are influenced by hormones known as androgens, which are present in both men and women but at different levels.
One androgen in particular plays a key role in pattern hair loss. In susceptible individuals, this hormone affects certain follicles in a way that gradually alters their function.
Over time, the affected follicles begin to produce thinner hairs during each growth cycle. The growth phase also becomes shorter, meaning the hair does not grow as long or as thick as it once did.
These changes do not occur simultaneously across all follicles. Instead, they develop gradually in specific regions of the scalp.
Follicle miniaturisation
One of the defining features of androgenetic alopecia is follicle miniaturisation.
Miniaturisation refers to the gradual shrinking of the hair follicle. As the follicle becomes smaller, the hair shaft it produces also becomes thinner.
During the early stages of this process, the changes may be subtle. A hair that was once thick may become slightly finer during the next growth cycle.
Over multiple cycles, the follicle may continue to shrink and produce increasingly thin hairs. Eventually, some follicles may produce very fine hairs that resemble the small, lightly pigmented hairs normally found on other parts of the body.
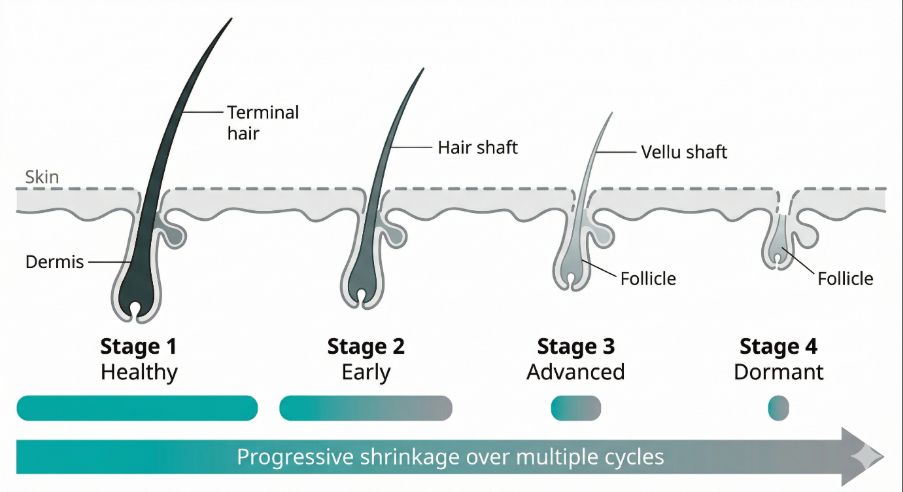
This gradual transformation from thick terminal hair to fine hair contributes to the visible thinning associated with male pattern hair loss.
Why certain areas of the scalp are affected
Male pattern hair loss does not affect all areas of the scalp equally.
Follicles at the temples and the crown are often more sensitive to hormonal signals in genetically susceptible individuals. These follicles are therefore more likely to undergo miniaturisation over time.
In contrast, follicles on the sides and back of the scalp are typically less sensitive to these signals. As a result, they often continue to produce thicker hair even when thinning occurs elsewhere.
This difference in follicle behaviour creates the characteristic patterns of hair loss seen in men.
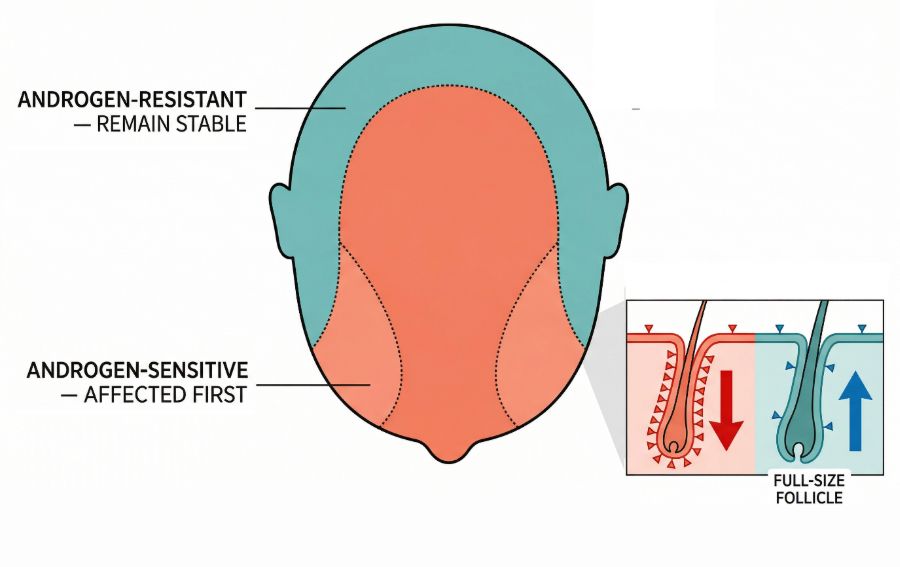
The progression of hair thinning
Male pattern hair loss usually progresses slowly.
In the early stages, individuals may notice a slight recession at the temples or mild thinning near the crown. Over time, these areas may become more pronounced as additional follicles undergo miniaturisation.
Because the process occurs over many growth cycles, visible changes may develop gradually over several years.
The patterns of progression are commonly described using classification systems such as the Norwood scale, which outlines different stages of hair thinning.
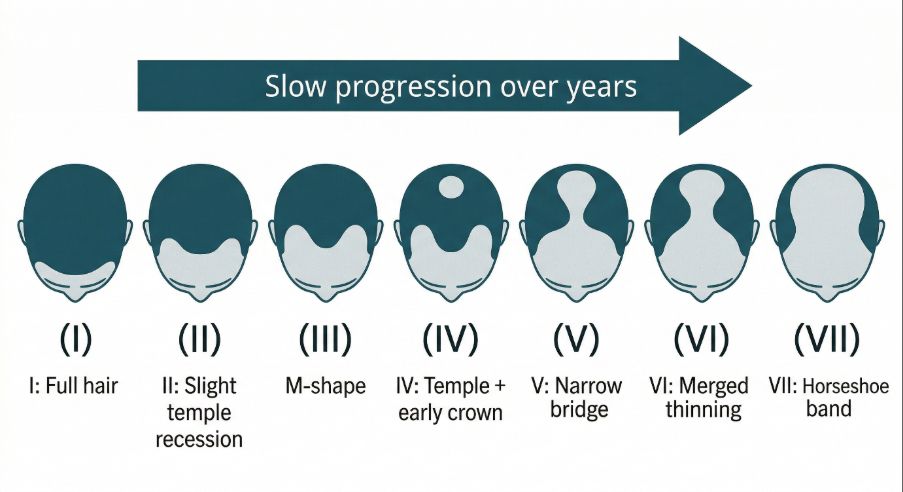
Changes in the hair growth cycle
Another feature of androgenetic alopecia involves changes in the hair growth cycle. Each follicle passes through three phases — anagen, catagen, and telogen — and in affected follicles the balance of these phases shifts over time.
Each hair follicle on the scalp operates within a repeating three-phase biological cycle that governs how long and thick the hair can grow, and when it is shed.
The anagen phase is the active growth period, lasting two to six years on the scalp. The duration of this phase directly determines the length and thickness of the hair shaft. Approximately 85 to 90 percent of scalp hairs are in anagen at any given moment.
The catagen phase is a brief transitional period of approximately two to three weeks, during which the follicle shrinks and detaches from its blood supply.
The telogen phase is the resting period, lasting approximately three months, after which the hair is shed and the follicle re-enters anagen to begin a new cycle. Because follicles cycle independently of one another, shedding is distributed gradually throughout the day rather than occurring all at once.
When hair loss becomes noticeable
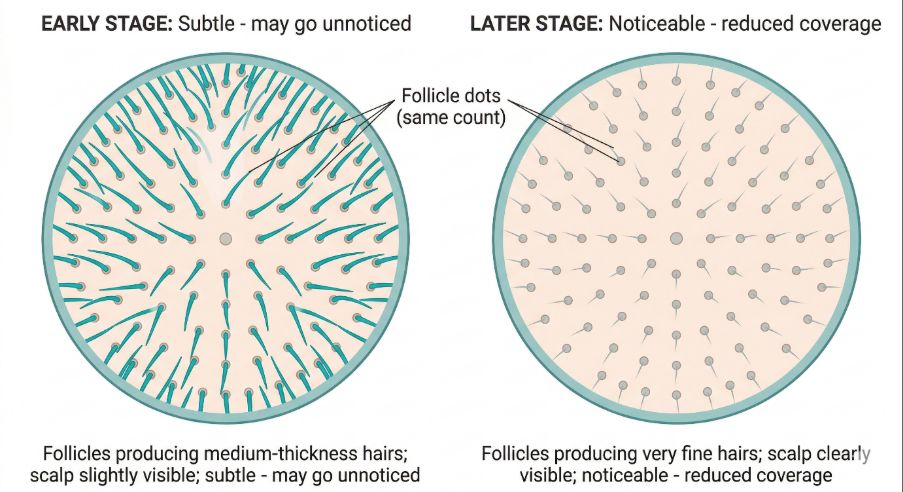
Hair thinning becomes noticeable when enough follicles have undergone miniaturisation to reduce overall hair coverage.
Because each follicle changes gradually, the early stages may be subtle. Some individuals first notice increased scalp visibility under bright light or when the hair is wet.
As the process continues, the pattern of thinning may become easier to recognise.
It is important to note that the number of follicles on the scalp usually does not change significantly. Instead, the follicles produce thinner hairs that provide less visible coverage.
Medications and chemical exposure
Certain medications can disrupt the hair growth cycle and contribute to hair loss or thinning. Drug categories known to affect the follicle include anticoagulants such as heparin and warfarin, antihypertensive agents including beta-blockers, retinoids, hormonal treatments, and oncology drugs. Cytotoxic chemotherapy agents are particularly notable — they can directly impair the anagen phase, causing rapid and pronounced hair loss within weeks of treatment beginning.
Chemical exposures are a further recognised cause. Heavy metals including thallium, arsenic, and mercury can damage follicle function, with exposure occurring through occupational contact, contaminated environments, or ingestion. Industrial solvents and aggressive chemical hair treatments may similarly impair follicle health. Identifying and removing the causative substance is the primary step toward allowing the hair cycle to normalise.
Differences between individuals
Male pattern hair loss can vary widely between individuals.
Some men experience only mild recession of the hairline throughout life. Others may develop more extensive thinning involving both the temples and the crown.
The age at which thinning begins also varies. In some cases the process starts in early adulthood, while in others it may begin later in life.
These differences reflect variations in genetic background and follicle sensitivity.
What research continues to explore
Although the general mechanisms behind male pattern hair loss are well recognised, researchers continue to investigate the detailed biological processes involved.
Scientists are studying how genetic factors influence follicle sensitivity, how hormonal signals affect follicle activity, and how the surrounding environment of the follicle contributes to the miniaturisation process.
Understanding these mechanisms may lead to improved strategies for managing hair loss conditions in the future.
A clinical perspective
Male pattern hair loss develops through gradual changes in the behaviour of hair follicles. In genetically susceptible individuals, certain follicles become increasingly sensitive to hormonal signals.
Over time these follicles shrink and produce thinner hairs during each growth cycle. Because this process occurs gradually and affects specific areas of the scalp, the condition develops in characteristic patterns.
Understanding these biological changes helps explain why male pattern hair loss progresses slowly and why it follows recognisable stages over time.
Author: Dr. Priya Goswami
Medical review: Dr. Denis Broun
Next step
If you notice coverage changes without increased shedding, confirm what process is occurring.
Take the Hair Assessment to have a physician review your pattern, identify whether miniaturization is present, and determine appropriate staging and next steps.

Add Comment